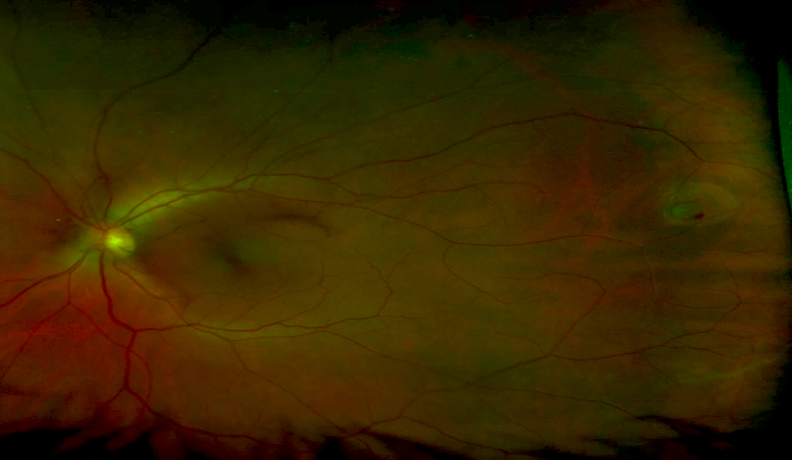
After surgery, patients must position themselves face down, as instructed by the surgeon, to allow the hole to heal completely. This procedure is performed in the outpatient setting under local anesthesia either in a surgery center or hospital. The surgery involves vitrectomy, or separation and removal of the vitreous gel from the eye with injection of a gas bubble within the eye. Typically, smaller macular holes with a short duration of symptoms and limited vision loss have the best results with treatment. The level of vision improvement and final result depend on the size of the hole, duration of symptoms, and the level of vision loss before surgery is performed. Macular holes can be closed surgically and successfully treated in approximately 90-95% of cases. Each stage can progress to the next if not treated. There are four stages of a macular hole: small foveal detachments with a partial-thickness defect (stage 1), small full-thickness holes (stage 2), larger full-thickness holes without vitreous separation from the retina (stage 3), and larger full-thickness holes with vitreous separation (stage 4). Peripheral vision usually is not affected, although in very rare instances such holes can cause retinal detachment. As the hole grows over several weeks or months, central vision progressively worsens. Most cases occur in people over the age of 60.Īt first, a macular hole may only cause a small blurry or distorted area in the center of vision. 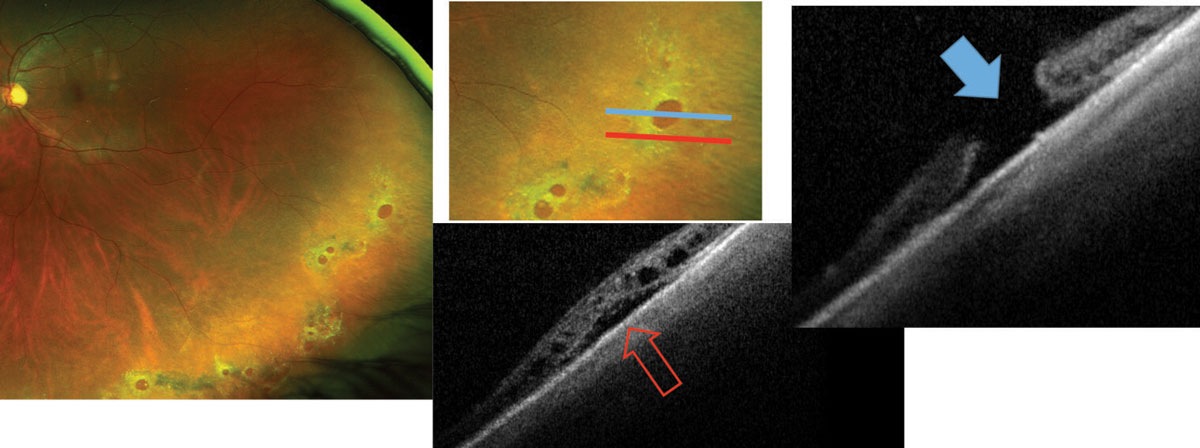
Less commonly, macular holes are caused by direct, blunt eye injury or can occur with intraocular inflammation, macular pucker, or retinal detachment. Rather than separating cleanly, the vitreous may abnormally stick to and pull on the macula causing a hole to form. 2012 32:1525–30.Macular holes most commonly develop spontaneously during the natural aging process, when the vitreous (the gel that fills most of the eye) becomes more like a watery liquid and separates from the retina. 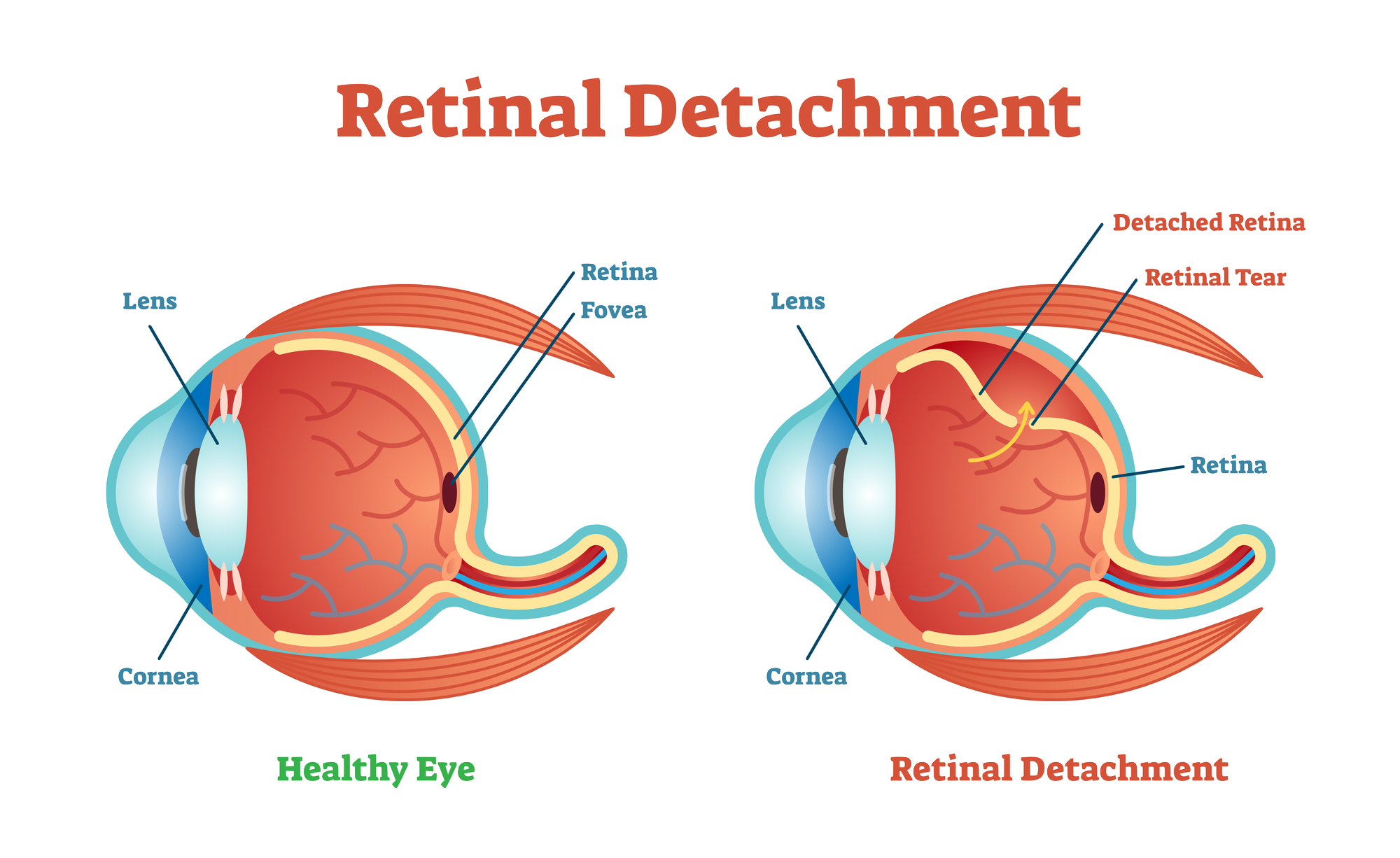
Treatment of retinal detachment secondary to macular hole in high myopia. Prognostic factor analysis in pars plana vitrectomy for retinal detachment attributable to macular hole in high myopia: a multicenter study. Nakanishi H, Kuriyama S, Saito I, Okada M, Kita M, Kurimoto Y, Kimura H, Takagi H, Yoshimura N. Pars plana vitrectomy and perfluoropropane (C3F8) tamponade for retinal detachment due to myopic macular hole: a prognostic factor analysis. Lam RF, Lai WW, Cheung BTO, Yuen CYF, Wong T, Shanmugam MP, Lam DSC. Optical coherence tomographic findings of macular holes and retinal detachment after vitrectomy in highly myopic eyes. Ikuno Y, Sayanagi K, Oshima T, Gomi F, Kusaka S, Kamei M, Ohji M, Fujikado T, Tano Y. A human amniotic membrane plug to repair retinal detachment associated with large macular tear. 2017 37:466–71.Ĭaporossi T, Tartaro R, de Angelis L, Pacini B, Rizzo S. Efficacy of the inverted internal limiting membrane flap technique with vitrectomy for retinal detachment associated with myopic macular holes. īaba R, Wakabayashi Y, Umazume K, Ishikawa T, Yagi H, Muramatsu D, Goto H. Treatment of macular hole retinal detachment with macular plug in highly myopic eyes: three-year results. Wu AL, Ling KP, Chuang LH, Chen KJ, Chen YP, Yeung L, Wang NK, Liu L, Chen TL, Hwang YS, Wu WC, Lai CC. Inverted internal limiting membrane flap technique as a useful procedure for macular hole-associated retinal detachment in highly myopic eyes. Sasaki H, Shiono A, Kogo J, Yomoda R, Munemasa Y, Syoda M, Otake H, Kurihara H, Kitaoka Y, Takagi H. Long-term outcomes of macular hole retinal detachment in highly myopic eyes after surgical reattachment. Kim HY, Lee JJ, Kwon HJ, Park SW, Lee JE. Macular hole closure over residual subretinal fluid by an inverted internal limiting membrane flap technique in patients with macular hole retinal detachment in high myopia. Okuda T, Higashide T, Kobayashi K, Ikuno Y, Sugiyama K. 
Extramacular drainage of subretinal fluid during vitrectomy for macular hole retinal detachment in high myopia. Jeon HS, Byon IS, Park SW, Lee JE, Oum BS. Myopic maculopathy: current status and proposal for a new classification and grading system (ATN). Ruiz-Medrano J, Montero JA, Flores-Moreno I, Arias L, García-Layana A, Ruiz-Moreno JM. ILM peeling in macular hole retinal detachment: insert or not? Graefes Arch Clin Exp Ophthalmol. Vitrectomy with internal limiting membrane peeling versus inverted internal limiting membrane flap technique for macular hole-induced retinal detachment: a systematic review of literature and meta-analysis. Yuan J, Zhang L-L, Lu Y-J, Han M-Y, Yu A-H, Cai X-J. Perfluorocarbon liquid-assisted neurosensory retinal free flap for complicated macular hole coexisting with retinal detachment.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
